Context & Background
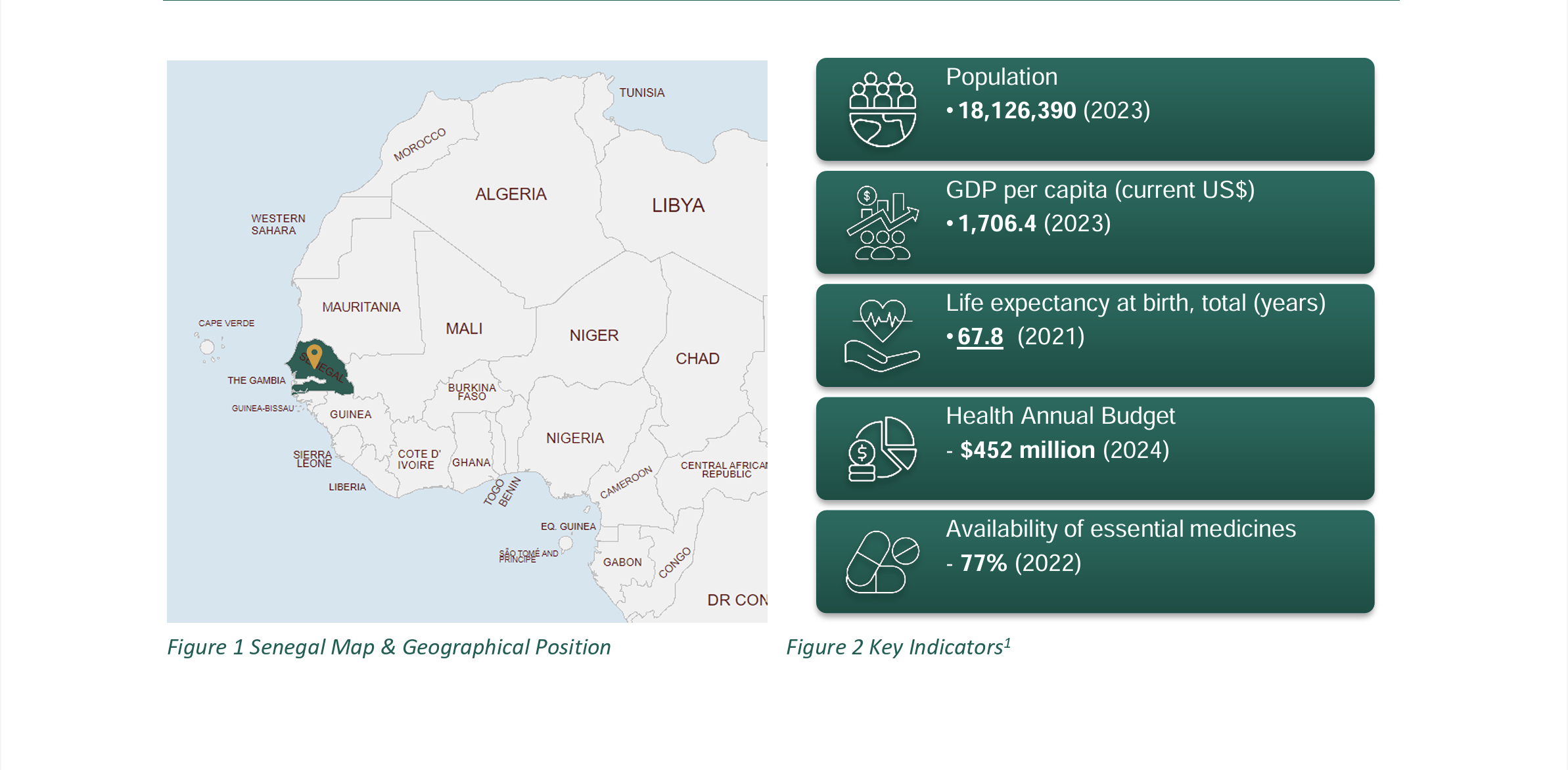
Equitable access to quality health services is a top priority for the Ministry of Health and Social Action (MoH) through the National Health and Social Development Plan (PNDSS). It reflects Senegal's ambition for Universal Health Coverage (UHC) and its implementation is oriented around three (03) axes: governance and financing, provision of health and social action services, and social protection.
The Ministry of Health has made considerable efforts to ensure the availability of medicines and health products through the strengthening of last mile distribution. The adoption of the Jegesi naa (region to district) and the Yeksina (district to service delivery point) distribution models has successfully allowed reduce stock-outs of family planning products. Unfortunately, due to the complexity of funding mechanisms and lack of strategic coordination and supply chain planning, the Yeksina model experienced malfunctions leading to its stoppage in 2019.
ARC’s assessment of Yeksi Naa operating and financial model in 2019 and the complementary studies conducted in 2021, extended to the entire supply chain, highlighted several challenges and constraints including:
- Lack of strategic coordination and centralized supply chain planning,
- Unharmonized supply chain information systems,
- Insufficient qualified human resources in Supply Chain management,
- Poor performance management framework
- Limited visibility on Supply Chain costs and complex funding mechanisms.
The Ministry of Health, with the support of donors and partners, is committed to addressing these challenges for the successful and effective relaunch of Yeksina, and for the long-term transformation of the public health supply chain, in alignment with the emerging development of local manufacturing.
Objectives of ARC interventions
In Senegal, by 2025, ARC's main mission is to assist the MoH in the implementation of recommendations from the Yeksi Naa evaluation, leading to a national strategy for public health supply chain in support of universal health coverage policies.
Indeed, ARC’s assessment of Yeksi Naa operating and financial model in 2019 and the complementary studies conducted in 2021, extended to the entire supply chain, highlighted several challenges and constraints.
As a result of the studies, ARC developed a roadmap for the relaunch of Yeksi Naa for a duration of one year and a 5-year roadmap for the long-term transformation of public health supply chain that will ensure the sustainability of supply chain initiatives.
Additionally, ARC agreed with MoH on key prerequisites to the relaunch that include:
- The setting up of PHSC governance entities for PHSC strategic coordination and decision-making,
- The development of a national PHSC strategy to define a strategic framework for the coordination of all supply chain programs, projects and investments for the strengthening of Public Health Supply Chain,
- The setting up of the strategic planning functions that include:
- The strengthening of processes and procedures (Sales & Operations Planning model) to optimize planning processes and ensure accurate forecasting,
- The reinforcement of human resources with the integration of supply chain profiles (to enable knowledge and competence transfer),
- The harmonization of information systems (logistics data management) for improved data availability and visibility for proper planning.
The Ministry of Health and partners requested ARC’s support for the implementation of the relaunch of Yeksi Naa roadmap and ARC is the focal point of partners as it relates to activities pertaining to the Yeksi Naa roadmap, under the lead of WHO
Expected Results
The expected results of the ARC intervention in Senegal are primarily to support and enable the long-term transformation of the Public Health Supply Chain through the improvement of supply chain sustainability with:
- A national health supply chain strategy will be a critical lever for achieving the universal health coverage goals in the country.
- New approaches (model design) to transform the supply chain with a specific focus on planning and operational distribution for last-mile delivery, supported by a sustainable funding mechanism.
- Enhanced functional multi-stakeholder supply chain governance structure, that should be based on a full, time-bound accountability framework for stakeholders, capable of effectively managing and implementing strategies.
- Improved visibility on the entire public health supply chain through better information systems enabled by routinely available data that is frequently collected and analysed to support evidence-based decision-making.






